The COVID-19 Vaccine Divide, Part 1: Perceptions & Effectiveness

Stories about COVID-19 breakthrough cases, safety of vaccines, mandates, booster shots, and so much more have been circling in the news and social media.
Partisan interests, bias by omission and misinterpretation of information make it tough to assess the COVID-19 vaccine's effectiveness with an objective lens. This is part 1 of a series devoted to breaking down COVID-19 vaccines and providing some perspective to the divide.
The U.S. Census Bureau estimates that as of September 20th, over 80% of U.S. adults received at least one dose of a COVID-19 vaccine. Democrats, college graduates, and elderly people are the most likely to have been vaccinated. Republicans are the least likely – as of September 20, nearly 1 in 4 Republicans say they will ‘definitely not’ get vaccinated.

A Pew Research Center (Center) survey in August found that nearly half of Americans (48%) receive at least some COVID-19 news and information on social media. Less than one-third say they have been getting no news or information at all. And with polarization being essentially built into social media, we’d argue it’s clear how much of an impact competing information has had on perceptions of vaccines – by keeping people in their filter bubbles and away from information they might disagree with, even if it’s accurate.
Overall, over 70% of Americans are confident the COVID-19 vaccines are safe and effective. There is a large divide, however, among vaccinated and unvaccinated adults: while almost 9 in 10 of vaccinated adults believe the vaccines are safe, just over 1 in 4 unvaccinated adults agree.
Many unvaccinated people are skeptical about the COVID-19 vaccines because of beliefs they are unsafe and ineffective. Vaccinated people are likely to report the exact opposite: they are more likely to report feeling safe, relieved, and protected.
Perception of vaccine side effects is so strong that 91% of people who say they won’t get vaccinated believe that the vaccine is a greater risk than possibly contracting COVID-19 itself.

Before we jump into the data available on vaccine effectiveness, it’s important to point out that some Americans (about 20%) have little to no trust in the federal government. And 34% of unvaccinated people say it’s a driving force behind not getting a shot. A YouGov survey conducted in September found that majorities of unvaccinated people don’t trust the medical advice from institutions like the CDC (57%) or FDA (52%). The reasons behind lack of trust in U.S. institutions are myriad and worth exploring, but not something we will delve into in this part of the series.
Some are more interested in alternative treatment protocols for COVID-19, which tend to include things like monoclonal antibodies, Vitamin D, and ivermectin; the newness of the vaccines are also a major driving factor in hesitancy. However, the FDA and other institutions do not recommend ivermectin for COVID-19 treatment. Read more about the debate over alternative treatments like ivermectin here.
The Centers for Disease Control and Prevention (CDC) reports that people who are not fully vaccinated are 4.5 times more likely to be infected, 10 times more likely to be hospitalized, and 11 times more likely to die from COVID-19 than those who are fully vaccinated. This study, conducted in recent months during the spread of the Delta variant, showed a rise in the rate of infection among both unvaccinated and fully vaccinated people, and a rise in the hospitalization and death rate driven primarily by the unvaccinated population.
According to CDC data, the COVID-19 vaccines appear to be extremely effective in preventing hospitalizations and deaths – much more than they are at preventing breakthrough cases – especially in the midst of the highly-transmissible Delta variant, which has been attributed to more than 99% of COVID-19 cases in the U.S. since mid-August.
Many on the left argue that the effects of the Delta variant would likely have been suppressed if more people were vaccinated and mask or vaccine mandates were implemented to a greater extent. On the right, arguments are sometimes made about questionable vaccine effectiveness, potential side effects such as myocarditis, and low hospitalization and death counts among healthy people.
If you’ve been following news about COVID-19, you’ve likely heard numbers pertaining to the efficacy or effectiveness of vaccines — such as that the Moderna and Pfizer vaccines had a 94% and 95% efficacy in clinical trials at preventing infection, respectively.
But these numbers are from clinical trials, and as with most vaccines, clinical trials often differ from real-world effectiveness of the vaccine. A recent study from the CDC shows that the effectiveness of the Pfizer and Moderna COVID-19 vaccines at preventing infection fell about 24% – from 90% to 66% – once the Delta variant became the predominant stain of COVID-19 in the U.S.
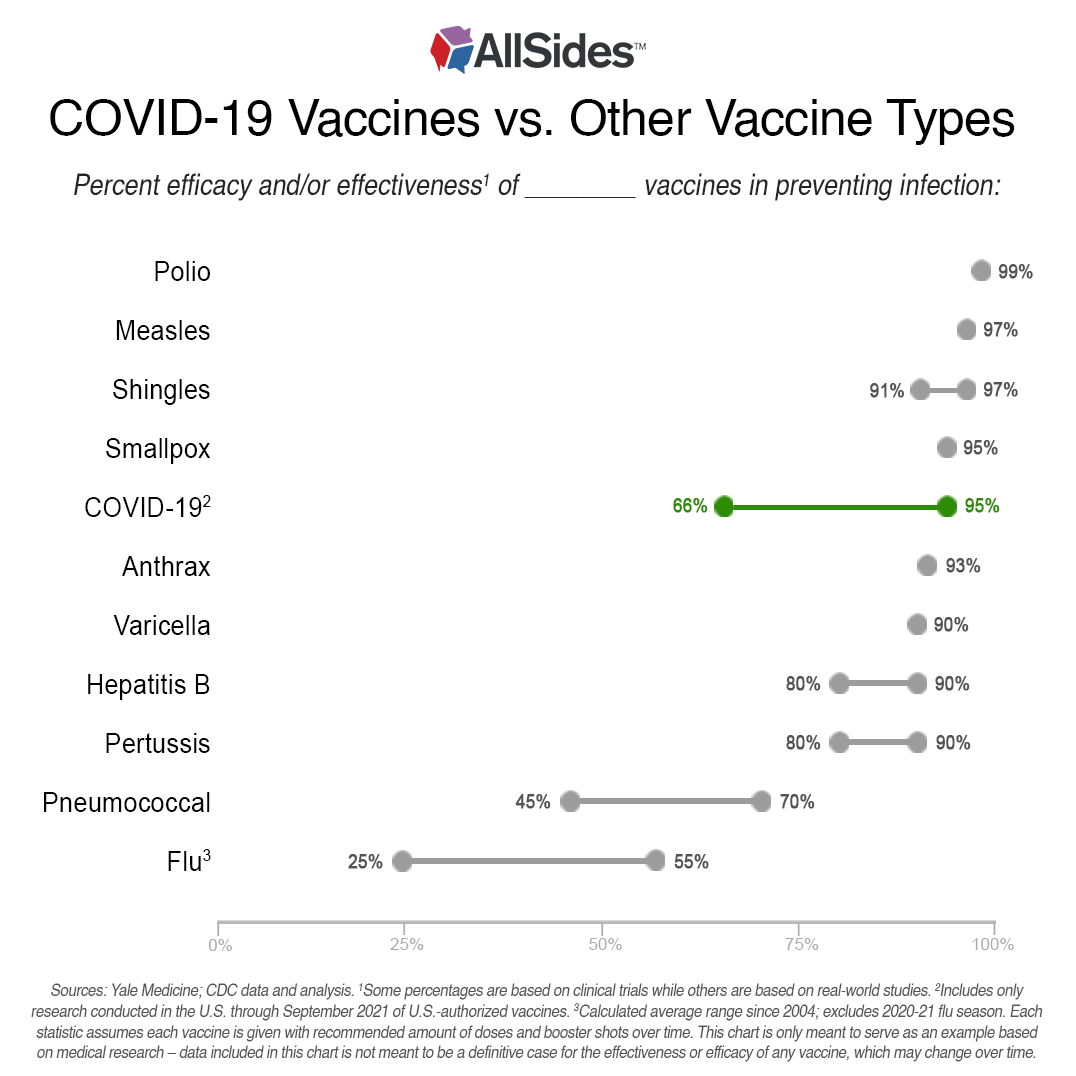
COVID-19 appears to be more effective in clinical trials than in real-world conditions, and recent research suggests it is mostly effective in preventing COVID-19 infection and very effective in preventing hospitalization and death among all demographics.
A vaccine effectiveness of 66% percent means that for every three unvaccinated Americans who are infected with COVID-19, two vaccinated people are spared an infection, on average, if both groups are exposed to the virus at the same rate. Many vaccines, like COVID-19 vaccines, have a waning effect over time. Only time, and the availability of booster shots, will tell how effective the vaccines are in the long-run.
The U.S. Department of Human Services (HHS) argued in August that “a booster shot will be needed to maximize vaccine-induced protection and prolong its durability.” The CDC found that Moderna and Pfizer vaccines were just 53% effective against infection among nursing home residents in June–July 2021, a decline from 75% effectiveness seen in March–May 2021.
As of September 30th, more than 184 million people in the U.S. have been fully vaccinated against COVID-19. And while there have been over 100,000 breakthrough cases of COVID-19, there have also been nearly 5,000 deaths, 86% of whom were adults aged 65 or older. However, CDC data also suggests that upwards of around 20% of these deaths were asymptomatic or not COVID-19 related at all, meaning that this number may be less than perceived (or more, if you believe that some COVID-19 deaths aren’t counted). In the same time frame, about 14,000 people were hospitalized with breakthrough cases.
In part 2 of this series on COVID-19 vaccines, we’ll break down studies on vaccine vs. natural immunity and look at the safety of the vaccines.
You can use AllSides to find more perspectives on the COVID-19 pandemic and COVID-19 vaccines.
Andrew Weinzierl is AllSides’ Research Assistant and Data Journalist. He has a Lean Left bias.
This piece was reviewed by Managing Editor Henry A. Brechter (Center bias) and Julie Mastrine, Director of Marketing and Bias Ratings (Lean Right).

April 22nd, 2024

April 19th, 2024

April 19th, 2024

April 18th, 2024